Pathophysiology of a Pneumothorax Case Study Order Instructions: Case Study-MRS. Richards
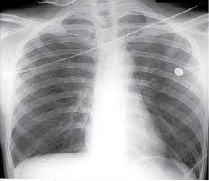
Mrs. Richards, daughter is a second-year student nurse. She tells you she doesn’t understand the pathophysiology of pneumothorax and why they can develop into a tension pneumothorax without UWSD(Underwater seal drain) insertion. Please explain to her the pathophysiology of pneumothorax and the UWSD and how it affects the cardiac & respiratory system using the correct medical and nursing terminology. the Assessment criteria below must be met in regards to this.
Pathophysiology of a Pneumothorax Case Study Assessment Criteria
1. We are to give a detailed explanation of the pathophysiology of the illness/disease of the case-patient, MRS Richards.
2. Explanation of 2 signs/symptoms the case-patient presented with and why they manifested as part of the illness/disease. The two sign and symptom Mrs. Richards had presented were chest tightness and shortness of breath.
3. Critical thinking and rationale – The patient, Mrs. Richards, is on some Antibiotics (Metronidazole and Cephalothin). Link this medication, A&P, pathophysiology, context, and theory together and give detail description as to why the medication is being given to Mrs. Richards, in regards to her pneumothorax, chest drain (UWSD).
Lastly linking pharmacology to multiple parts of practice such as; infection control, safety, Nursing consideration.
P.S. Can you please attach/send me pdf copies of the articles used in your research for this paper because I will need to attach it to my original paper when submitting.
Pathophysiology of a Pneumothorax Case Study Sample Answer
Pneumothorax Case Study
Introduction
Pneumothorax is a medical condition where the pleural cavity gets filled with air, which impairs ventilation and oxygenation. This health complication occurs when air leaks in the pleural cavity (space between lungs and chest walls) which creates an external force outside (destroys negative pressure) the lungs making them collapse. It can be caused by chest injury or medical health disorders. This medical complication may occur in various clinical settings and in any person of any age (Tamburrini, Sellitri, Tacconi, Brancati & Mineo, 2015). This paper explores the disease pathophysiology and ways it with the disease clinical manifestation. The paper also critically analyses the medication to give detailed information on the rationale behind the administration of specific medication. The concepts of pharmacology will be linked to nursing practice such as patient safety and infection control.
Causes and risk factors
Pneumothorax is caused by many factors. To start with, the patient may experience chest injuries (blunt or penetrating) that occur during physical accidents or physical assaults. Others causes include pleural lacerations caused during the medical procedures such as inserting aspiration needles in the patient chest. Damaged lung tissues are likely to cause air leakages into the pleural cavity. Lung disorders can be caused by many underlying diseases such as pneumonia, cystic fibrosis or chronic pulmonary diseases. In some cases, small air blisters (blebs) can develop in the lungs, which could burst, causing air to leak into the spaces surrounding the lungs. There incidences when pneumothorax occurs in patients with breathing difficulty and who require mechanical assistance. The mechanical ventilation used can cause an imbalance of air pressure and could cause the lungs to collapse (Tamburrini, Sellitri, Tacconi, Brancati & Mineo, 2015).
The main risk factors associated with pneumothorax include gender, where men are more likely to suffer from pneumothorax as compared to women. The risk of pneumothorax increases with poor lifestyles such as smoking. Pneumothorax caused by ruptured air blisters is common in people between the ages of 20 years and 40 years, and common in tall and underweight people. Genetics also plays a huge role as it mainly appears in families with a history of pneumothorax. Other risk factor includes lung disorders and mechanical ventilation (Ling, Wu, Ming, Cai & Chen, 2015).
Pathophysiology and clinical manifestation
The pathophysiology of pneumothorax is described according to the causes. Traumatic pneumothorax occurs due to penetrative injuries such as the impaled object, gunshot wound, and stab wound which are associated with traumatic open pneumothorax closed pneumothorax or haemo-thorax of the pneumothorax. Traumatic open pneumothorax occurs when the pleura gets lacerated and allows accumulation of atmospheric air in the pleural cavity. Its mainly cause by penetrating chest trauma. Air in the pleural cavity interrupts normal negative pressure which makes the lungs not remain inflated. The traumatic closed pneumothorax occurs when laceration of the pleura is caused by blunt trauma, causing air to enter the pleural cavity (Tamburrini, Sellitri, Tacconi, Brancati & Mineo, 2015).
Latrogenic traumatic pneumothorax occurs when the pleura laceration is caused by therapeutic and diagnostic procedures such as needle biopsy, mechanical ventilation, central line insertion, and aspirations. Air trapped in a pleural cavity interrupts normal negative pressure which makes the lungs not remain inflated. Spontaneous pneumothorax is an example of a closed type. This is common in geriatric patients diagnosed with chronic pulmonary diseases but can also occur in adults. The main cause of pleura rapture is mainly underlying respiratory disorders such as asthma, pneumonia, chronic airflow limitation (CAL), tuberculosis, disorders of the connective tissues, Cystic fibrosis and Marfan’s syndrome.
Tension pneumothorax is caused by either traumatic of spontaneous pneumothorax. The pleura get raptured allowing air into the pleural cavity but do not allow it to escape. This creates tension and pressure in the intrapleural space, which makes the affected lung to collapse, squeezing the mediastinal contents to the unaffected lung. Air in the pleural cavity interrupts normal negative pressure which makes the lungs not remain inflated (Corsini, Pratesi & Dani, 2013).
The main clinical signs of pneumothorax are the sudden sharp pain around the chest, which is normally exacerbated by chest movements such as coughing and breathing. The asymmetrical chest movement causes the lungs to collapse. These results to cyanosis and shortness of breath associated with hypoxia. Other clinical manifestations include decreased vocal fremitus and respiratory distress, which are associated with collapsing of the lungs. When auscultation is done, the breath sounds on the side affected lung are absent as the lung has collapsed (Chiu, Chen, Wang, Tsai & Wong, 2014).
Chest rigidity on the affected side may occur due to tachycardia and hypoxia. Palpation of the affected side normally reveals crackling sound just beneath the skin, which is normally due to the leaking of air into the tissues. Research indicates that Tension Pneumothorax has the most severe clinical manifestation which includes hypotension, reduced cardiac output, tachypnea, and compensatory tachypnea. The disease diagnosis is normally done using X-rays, which is normally reveals air in the pleural space. Arterial blood analysis normally can be used to reveal hypoxemia (Lee et al., 2014).
Medical management and patient education
The main medical management is done by cutting through the chest (thoracotomy) is required. This is done by inserting a chest tube in the 5th and 6th intercostal space located under the patient’s arm. The tube is then attached to a water-seal drainage system, which drains all the air in the pleural cavity. The chest tube is normally a long hollow tube which is inserted as described above. This is normally done under local anesthesia (Gale et al., 2015).
The pleural space refers to the space between the visceral and parietal layers that line has inside the lungs and chest cavity. Normally, the two layers are held together by negative pressure or vacuum, which ensures that the lungs remain inflated. The pleural space is normally empty except the small amount of fluid that helps reduce friction between the cavities. In special cases, air or fluid may accumulate causing pneumonia, chest trauma or other intraabdominal conditions. Pneumothorax could also occur. This results to chest tightness and breathing difficulty (Baird & Gandhi, 2014).
The chest drains are done so long as air remains in the pleural cavity. This must be done because without UWSD, pneumothorax can result in a tension pneumothorax. This is because the air trapped in the pleural cavity prohibits air outflow. Consequently, the volume of the air in the pleural cavity increases with every inspiration causing the pressure in the pleural cavity to increase causing lungs to collapse. Further increase of pressure in the pleural cavity makes the mediastinum shift towards the contralateral side of the lungs, which obstructs the venous return to the heart. This causes circulatory instability and could result in a traumatic arrest. This is indicated by cardiovascular diseases, reduced oxygen, and low blood pressure. The patient needs to have regular chest X-rays and to monitor the disease progress (Curfman, Robitsek, Sammett & Schubl, 2015).
This intensive care is associated with potential risks and complications even when performed by experienced staff. The main common health complications are pain and infection. For example, drains inserted into the body increases the risks of infection. Therefore, the patients and patient relatives must not touch the drain, tubes and the dressings that cover the site of insertion. Good hygiene practices such as washing hands before and after contacting the patient also helps minimize patient’s risks of infection. Some degree of pain, infection control, and patient safety must be discussed by healthcare providers (AL Saif, Hammodi, Al-Azem & Al-Hubail, 2015).
The treatment of pneumothorax mainly depends on the size of the pneumothorax. Small pneumothorax normally resolves by its self. The aim of the treatment is to get rid of the accumulated air in the pleural space. Once the lungs are filled with air, the patient is able to breathe with ease. The patient is given Metronidazole and Cephalothin antibiotics in order to treat and prevent bacterial infection during UWSD procedures. The patient should also be given pain medication such as Tylenol. The pain prescription is done to decrease a patient’s pain. The pain medication should be done as directed. Sedative medication is given to make the patient remain calm and relaxed when performing needle aspirations and chest tubes (Dixit, Meena & Patil, 2015).
Pathophysiology of a Pneumothorax Case Study References
AL Saif, N., Hammodi, A., Al-Azem, M., & Al-Hubail, R. (2015). Tension Pneumothorax and Subcutaneous Emphysema Complicating Insertion of Nasogastric Tube. Case Reports in Critical Care, 2015, 1-4. http://dx.doi.org/10.1155/2015/690742
Baird, A., & Gandhi, M. (2014). Pneumopericardium and pneumothorax due to the right atrial permanent pacemaker lead perforation. Journal of Medical Imaging and Radiation Oncology, 59(1), 74-76. http://dx.doi.org/10.1111/1754-9485.12200
Chiu, C., Chen, T., Wang, C., Tsai, M., & Wong, K. (2014). Factors associated with proceeding to surgical intervention and recurrence of primary spontaneous pneumothorax in adolescent patients. European Journal of Pediatrics, 173(11), 1483-1490. http://dx.doi.org/10.1007/s00431-014-2352-0
Corsini, I., Pratesi, S., & Dani, C. (2013). Pulmonary interstitial emphysema after resolution of relapsing pneumothorax and discontinuation of mechanical ventilation. An atypical case in a preterm infant. The Journal of Maternal-Fetal & Neonatal Medicine, 27(15), 1610-1612. http://dx.doi.org/10.3109/14767058.2013.867322
Curfman, K., Robitsek, R., Sammett, D., & Schubl, S. (2015). Blunt trauma resulting in pneumothorax with progression to pneumoperitoneum: a unique diagnosis with the predicament in management. J. Surg. Case Rep., 2015(12), rjv147. http://dx.doi.org/10.1093/jscr/rjv147
Dixit, R., Meena, M., & Patil, C. (2015). Pneumomediastinum, bilateral pneumothorax and subcutaneous emphysema complicating acute silicosis. Int J Occup Med Environ Health, 2015(2). http://dx.doi.org/10.13075/ijomeh.1896.00399
Gale, M., Loarte, P., Mirrer, B., Mallet, T., Salciccioli, L., Petrie, A., & Cohen, R. (2015). Takotsubo Cardiomyopathy in the Setting of Tension Pneumothorax. Case Reports in Critical Care, 2015, 1-5. http://dx.doi.org/10.1155/2015/536931
Lee, K., Kim, K., Kim, E., Lee, J., Kim, Y., & Hyun, S. et al. (2014). Detection of blebs and bullae in patients with primary spontaneous pneumothorax by multi-detector CT reconstruction using different slice thicknesses. Journal of Medical Imaging and Radiation Oncology, 58(6), 663-667. http://dx.doi.org/10.1111/1754-9485.12229
Ling, Z., Wu, Y., Ming, M., Cai, S., & Chen, Y. (2015). The Effect of Pleural Abrasion on the Treatment of Primary Spontaneous Pneumothorax: A Systematic Review of Randomized Controlled Trials. PLOS ONE, 10(6), e0127857. http://dx.doi.org/10.1371/journal.pone.0127857
Tamburrini, A., Sellitri, F., Tacconi, F., Brancati, F., & Mineo, T. (2015). Simultaneous Bilateral Spontaneous Pneumothorax Revealed Birt-Hogg-Dubè Syndrome. Case Reports In Surgery, 2015, 1-3. http://dx.doi.org/10.1155/2015/916039




